Hair Transplant Recovery Timeline: Aftercare Day 1 to Month 12
What recovery from hair transplant actually looks like: day-by-day, week-by-week, month-by-month. When to wash, work, fly, exercise — and when to expect results.
Medical disclaimer. This article is educational and not medical advice. Hair restoration outcomes are individual; only a qualified surgeon can assess your case in a personal consultation.
Quick answer
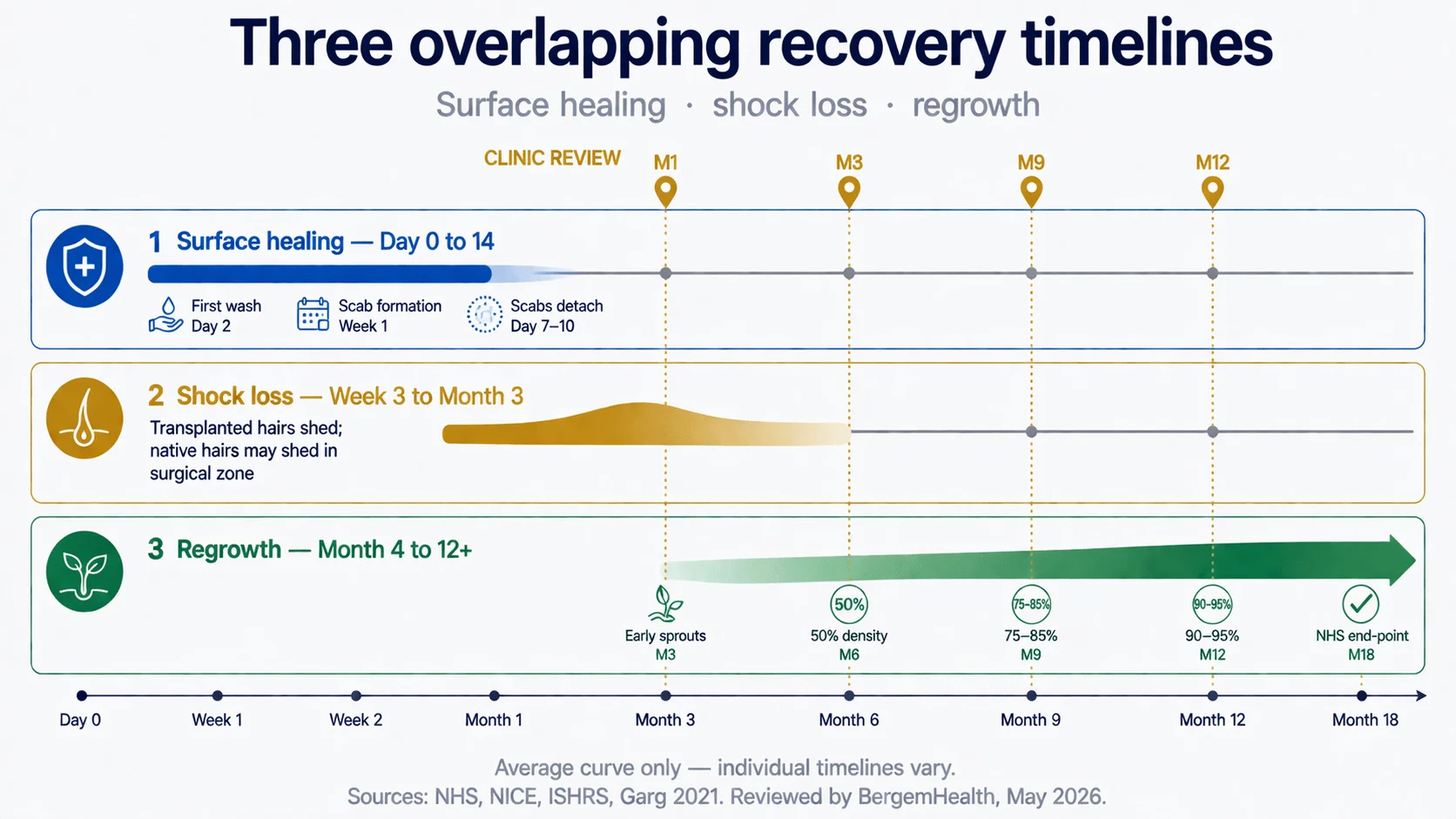
Hair transplant recovery happens on three overlapping timelines that patients tend to confuse. Surface healing — scabs, redness, swelling — is largely complete within 14 days. The shock-loss phase — when transplanted hairs shed before regrowing — runs from week 3 to month 3 and is when most patient anxiety peaks. Final-result emergence runs from month 4 through month 12, with month 12 the standard end-point for assessment and NHS guidance allowing up to 18 months for full maturationnhs. This guide walks each stage with what’s normal, what isn’t, and what to do at each point.
Table of contents
- The three recovery timelines
- Recovery planning before surgery
- Day 0 and the first 7 days
- Weeks 2–4 — surface recovery completes
- Months 1–3 — the shock-loss phase
- Months 3–6 — the awkward stage
- Months 6–12 — regrowth and final density
- Reconciling 9–12 months and the 18-month NHS review
- What to do (and not do) at each stage
- When to call the clinic
- How BergemHealth approaches aftercare
- What to do next
- Frequently asked questions
The three recovery timelines
Definition. Hair transplant recovery is the multi-stage biological process by which surgical sites heal, transplanted follicles establish themselves in their new location, and mature hair regrows. The process has three distinct phases that occur partly in parallel and partly in sequence.
The three phases:
| Phase | Timeframe | What’s happening |
|---|---|---|
| Surface healing | Day 0 to ~Day 14 | Donor and recipient sites scab over and heal; redness fades |
| Shock loss & dormancy | Week 3 to Month 3 | Transplanted hairs shed; follicles enter resting phase before regrowing |
| Regrowth & final density | Month 4 to Month 12 | Follicles produce mature hair shafts; visible density builds gradually |
The mistake most patients make is judging the result during phase 2. Month 2 — when the surface is healed but the transplanted hairs have shed and nothing has yet regrown — is the lowest visual point, and it’s where most “I think the surgery failed” anxiety happens. The result isn’t valid until phase 3 has completed, which means the 12-month milestone is the standard assessment point, not 2 months, not 6 monthsnhsstatpearls.
The biology underlying these phases is well documented. Modern FUE technique reports 90–95% graft survival when extraction, holding-solution time, and implantation are well controlledsharma. The follicles that survive almost always proceed through the same anagen-catagen-telogen cycle they followed before surgery, just on a synchronised timeline because they were all moved at once.
Recovery planning before surgery
Recovery should be planned before the operation date, not improvised afterwards. A practical pre-op plan answers a small list of concrete questions: who will drive or accompany you home from the clinic; when the first wash happens (and, for travel patients, when that wash falls relative to the return flight); how you will sleep semi-upright for the first 3–5 nights; when you can return to calls, meetings or office work; whether scabs and redness can be hidden under a loose cap during the recovery week; and what to do if swelling moves toward the eyes on day 2 or 3.
The plan should be written and specific. Patients should leave the clinic with medication instructions, washing steps, contact details, photo instructions and a clear list of symptoms that require same-day contact — not relying on memory after a long surgical day. Travel patients booked through Istanbul typically schedule the return flight from day 4 or later so the day-2 clinical wash, day-3 review and at least one supervised home wash all happen before departure.
Time off work to plan into the diary: a working week (5 working days) is the minimum for desk-based roles, two weeks more comfortable. Public-facing roles benefit from 10–14 days off because visible redness on the recipient area is normal through day 7–10. Physically demanding roles (construction, manual handling, anything that pulls heart rate above 100 bpm reliably) should plan 2–3 weeks before resuming and discuss specific tasks with the clinical team.
Day 0 and the first 7 days
Day 0 — the surgical day — is long but routine: total in-theatre time for a 2,500–3,500 graft case is typically 6–10 hours including breaks, with the surgeon personally performing extraction in surgeon-led practice. Patients leave with dressings on the donor area, a protective headband, a post-op medication pack (paracetamol or codeine, antibiotic prophylaxis depending on protocol, antihistamine for swelling), and written aftercare instructions. No driving on day 0. Sleep semi-upright using a travel pillow or stack of pillows for the first 3–5 nights to reduce overnight forehead swelling.
The first 7 days are detailed in the day-by-day cluster guide. The shape:
- Day 1: First clinic review, dressing check, photographs.
- Day 2: First wash demonstration at the clinic — staff perform the wash and show you the technique.
- Day 3: Continue daily wash protocol; mild forehead swelling may peak today; ice on the forehead helps but never on the recipient area.
- Day 4: Most desk-based workers return to work, often with a loose cap during the commute.
- Day 5: Crusts start to loosen; itching may begin (a normal sign of healing).
- Day 6: Crusts continue to detach. No scratching or picking — let them fall off naturally with washing.
- Day 7: First cosmetic milestone. Most surface crusts have detached.
Through this week: avoid alcohol entirely (interferes with healing and increases scalp blood flow), avoid smoking (constricts vessels new grafts need open to establish blood supply)statpearls, no gym or exercise that raises heart rate above 100 bpm.
Weeks 2–4 — surface recovery completes
By end of week 2, the surface picture is essentially normal:
- Donor area: small healing punch points, fading from red to pink, typically not noticeable from a normal social distance
- Recipient area: transplanted hairs visible as short stubble — donor-zone-quality hair embedded in the recipient area
- No scabs, no swelling, no significant redness in most patients
- Hair washing: returns to normal frequency and technique; gentle rubbing over the recipient area is now safe
This is also when the first sign of shock loss typically appears. Around week 3, patients start to notice transplanted hair shafts shedding — they appear in the shower, on the pillow, and on clothing. The follicles themselves are not lost; they’re entering a temporary resting (telogen) phase before the new growth cycle begins. The full discussion is in shock loss explained.
By end of week 4: most original transplanted hair shafts have shed. The surface looks similar to pre-surgery, except for the now-visible donor-area pattern (small areas of reduced density at the back/sides where grafts were extracted — visible to close inspection but not from normal distance).
What you can do at week 4:
- Resume regular gym if heart rate is monitored and comfortable (avoid exercises that put pressure on the recipient area)
- Resume swimming in chlorinated pools (sea/saltwater can wait until week 5–6)
- Resume light alcohol in moderation (heavy drinking still better avoided through month 1)
- Hat-wearing is fine throughout, including the first 4 weeks — just avoid tight-fitting hats that press on the recipient area in days 0–10
The activity-gating logic across the first 4 weeks reduces to two principles: don’t disturb the grafts mechanically, and don’t drive scalp blood flow excessively. Mechanical disturbance is why scratching, picking at crusts, tight hats, sea-swimming, contact sport and head-on-pillow side-sleeping are restricted in the first 7–10 days. Excessive scalp blood flow is why heart-rate-elevating exercise, hot saunas, alcohol and nicotine are restricted through weeks 1–2 — vasodilation in the early days can compromise the fragile new blood supply the grafts are establishingstatpearls.
Months 1–3 — the shock-loss phase
The most psychologically difficult period of recovery. By month 1, most transplanted hair shafts have shed. The recipient area looks similar to pre-surgery — bald or thinning in roughly the same pattern. Patients commonly experience: “the surgery hasn’t worked” anxiety, doubt about the decision, comparison to month-1 photos online (which often look worse than reality because patients posting at their lowest point dominate the visible content).
What’s actually happening biologically: the transplanted follicles are alive in the scalp but in the telogen (resting) phase. Hair production has stopped temporarily while the follicle re-establishes itself in its new blood supply. This typically lasts 8–12 weeks per follicle, with different follicles entering and exiting telogen at slightly different times — which is why regrowth doesn’t all happen at once.
By month 3:
- First new growth begins: thin, fine, often colourless hairs starting to push through. Sometimes called the “ugly duckling” stage because the new hairs are not yet at adult thickness or pigmentation.
- Density looks like roughly 5–15% of expected final result — visibly improved on the month-1 low point but nowhere near final
- Patient anxiety usually peaks between week 8 and week 12, then begins to resolve as new growth becomes visible
What to do during this phase: trust the timeline, take comparison photos at month 1 and month 3 in identical lighting, avoid the “I should be at month 12 by now” mental trap. The biology is fixed; the timeline is non-negotiable. (Detail in the month-by-month results article.)
Months 3–6 — the awkward stage
Months 3–6 are the visible regrowth phase. Each month adds noticeable density. The new hairs progress from:
- Month 3: thin, colourless, ~1 cm long
- Month 4: thicker, beginning to take on adult colour, ~2 cm long
- Month 5: closer to adult thickness, full pigmentation, ~3–4 cm
- Month 6: roughly 50% of the eventual final density is visible
The “awkward stage” name comes from the appearance during this period: new hairs are growing in unevenly because different follicles emerged from telogen at slightly different times. Patients often see patches of denser regrowth alongside sparser areas. By month 6 this evens out substantially.
Photographing yourself monthly during this phase is more useful than weekly checking — the changes are real but slow, and weekly comparison can feel discouraging where monthly comparison reveals clear progress. A consistent self-photography protocol (same fixed location, same overhead light, same five angles, same dry-and-unstyled hair state, same camera in default mode) is one of the most useful things a patient can do across the 12-month recovery — full protocol in the month-by-month results article.
Months 6–12 — regrowth and final density
This is the phase when results fully resolve. The trajectory:
- Month 6: 50% of final density visible
- Month 7–8: 60–70%
- Month 9: 75–85% — touch-up assessment point if density is below the agreed threshold
- Month 10–11: 85–95%
- Month 12: 90–95%+ — the standard assessment point
The follicles that have grown by month 12 are biologically the donor-zone follicles, retaining their DHT-resistance and continuing to grow throughout life — that’s the basis of why hair transplant produces durable results, with the caveat that native hairs in the surrounding AGA-affected zone can still recede, which is why most surgeons recommend continuing finasteride and/or minoxidil to protect native density (see the AGA article). The transplant addresses density in the affected zones at the time of surgery; medical management around the transplant zones addresses the trajectory of the surrounding native hair.
Reconciling 9–12 months and the 18-month NHS review
Two timeframes appear in patient information and they can look contradictory: 9–12 months for “final result” and 18 months in NHS cosmetic-surgery guidance. They aren’t in conflict.
Most patients see effectively their final result by month 9–12 — by that point density is at 90–95%+ of the eventual outcome and the picture is stable enough for honest assessment. NHS guidance allows up to 18 months for full maturation, which is the formal end-point for cosmetic-surgery reviewnhs. The extra 6 months between month 12 and month 18 typically delivers a small additional percentage of density (around 5%) and lets the donor-area healing and any native-hair shock-loss recovery fully stabilise.
For practical purposes: the surgical outcome can be honestly evaluated at month 12. The 18-month NHS frame is the formal long-term review point and confirms result durability rather than further regrowth.
Patients sometimes interpret “wait until 18 months” as a signal that the result might still meaningfully change between month 12 and month 18 — it usually doesn’t. The 18-month figure exists because cosmetic-surgery outcome reviews need a durability check rather than because regrowth continues meaningfully past month 12. If your month-12 review shows the agreed target density and a stable picture, the month-18 review is a confirmation, not a course correction.
What to do (and not do) at each stage
A consolidated do/don’t reference. Specific aftercare protocols vary slightly by clinic — always follow your clinic’s specific instructions over generic guidance.
| Stage | Do | Don’t |
|---|---|---|
| Day 0–3 | Sleep semi-upright; take prescribed medication on schedule; ice forehead (not recipient area) for swelling | Drive on day 0; bend over; lift anything heavy; touch the recipient area unnecessarily |
| Day 4–7 | Begin daily wash protocol; return to desk work if comfortable; cover with loose hat if needed | Pick at scabs; scratch the recipient area; use harsh products; consume alcohol |
| Week 2–4 | Resume normal washing technique; gentle social activities; cap-wearing if preferred | Swim in sea/saltwater; do contact sport; expose to direct sunlight without protection |
| Month 1–3 | Trust the timeline; photograph monthly; continue prescribed medications | Compare to others’ month-1 photos online; assume the surgery has failed; restart heavy alcohol |
| Month 3–6 | Photograph monthly; resume full exercise routine; continue medications | Judge the final result yet; expect even regrowth (it’s uneven during this stage) |
| Month 6–12 | Photograph monthly; attend scheduled review appointments | Assume month 6 = final result; skip touch-up review at month 9 if offered |
When to call the clinic
Most aftercare unfolds without complications. Some signs do warrant same-day clinic contact:
| Symptom | Timeframe | Action |
|---|---|---|
| Severe pain not controlled by paracetamol/codeine | Any time | Same-day call |
| Spreading redness beyond the surgical sites | Day 1+ | Same-day call (possible infection) |
| Pus or discharge from any surgical site | Day 1+ | Same-day call |
| Fever above 38°C | Day 1+ | Same-day call |
| Unusual swelling beyond expected day-2/3 forehead swelling | Day 1+ | Same-day call |
| Bleeding from the donor area that doesn’t stop with gentle pressure | Day 1+ | Same-day call |
| Worsening scabs or scab patterns that don’t match described expectations | Week 1+ | Photograph and message the clinic |
| No regrowth visible at month 4+ | Month 4+ | Schedule a clinic review (likely normal but worth confirming) |
The published complication-rate literature for hair transplant under local anaesthesia in regulated settings reports rates well under 1% for serious adverse events, with the most common minor issues being folliculitis (small infected follicles, treatable with antibiotics) and temporary numbness in the donor areagarg. Most concerns patients raise turn out to be normal-but-frightening features of healing rather than complications — but the threshold for calling should be low. A clinic that returns calls promptly and engages with the photographs you send is doing the right thing; one that makes you feel you’re being inconvenient is not.
How BergemHealth approaches aftercare
BergemHealth includes a 12-month aftercare bundle at both Liv Hospital Ulus, Istanbul and 99 Harley Street, London — same protocol, same case-record format, same touch-up policy regardless of which pathway the patient chose. Structured reviews fall at month 1, 3, 6, 9 and 12, with format varying by location:
- London pathway: in-person reviews at 99 Harley Street with the GMC-registered consulting teamgmc. ~30 minute appointments; clinical examination, density mapping, photographs added to the patient’s case record.
- Istanbul pathway: remote reviews via high-resolution photo and video upload, plus video call with the clinical team. Patients who want in-person review can do so at Harley Street as a no-additional-fee service since the clinical network is shared.
The touch-up policy is defined in writing in the booking documentation: if month-9 density falls below an agreed threshold, a corrective procedure is performed at no additional surgeon fee at either clinic. The “agreed threshold” is graft count and density expectations established in the pre-op consultation, not a vague “we’ll see how it looks” assurance — that distinction matters because well-defined language gives patients a clear consumer-protection floor.
In practice, the patients who use the touch-up policy are typically those whose regrowth at month 9 is at the low end of the expected range — in our experience, around 5–10% of cases. The majority reach month 12 with results within the expected range and don’t need additional surgery. The aftercare structure is the same whether the original surgery was performed in Istanbul or London: same review schedule, same case-record format, same touch-up threshold, same access to the clinical team via the message channel between scheduled reviews.
Dr. Hamid Aydın leads the surgical pathway at Liv Hospital Ulus (ISHRS member, 25,000+ procedures since 2000)ishrs; Dr. Sumeyye Yuksel leads the London consulting and aftercare teamgmc. Both clinics share the same aftercare bundle, the same threshold-based touch-up policy and the same monthly review cadence, so patient experience after surgery is consistent regardless of which pathway was chosen for the procedure itself.
What to do next
For the immediate post-op week, see first 7 days after FUE day-by-day. For the month-by-month timeline with what to expect at each milestone, the month-by-month results article. For the shock-loss phase specifically — the period that causes the most patient anxiety — shock loss explained.
For surgical-method choice (which affects recovery timeline modestly — Sapphire FUE typically heals 1–2 days faster than Standard FUE; Direct DHI similar), see the methods comparison and the hair-transplant pillar.
If you’re considering surgery and want to understand the recovery commitment before booking, request a free assessment from BergemHealth’s London or Istanbul team. The consultation walks through realistic recovery expectations, the 12-month aftercare programme, and the touch-up policy in writing. CQC-registered facility in London. JCI-accredited hospital in Istanbul. ISHRS-member lead surgeon.
Frequently asked questions
How long is hair transplant recovery overall?
Surface recovery: 14 days. Most patients are back to normal social and work life by day 7–14. The shock-loss phase ends around month 3. Final density emerges between month 6 and month 12, with month 12 the standard assessment point and NHS guidance allowing up to 18 months for full maturationnhs. So “recovery” is 12 months if you mean reaching final result; 14 days if you mean returning to normal life.
When can I wash my hair after a hair transplant?
The first wash is typically performed at the clinic on day 1 or 2 post-op as a demonstration. From day 2 onward, most clinics issue a daily home-wash protocol using a specific saline solution and gentle shampoo. Normal washing technique resumes around day 14 once all crusts have detached. Specifics vary by clinic — follow your clinic’s instructions.
When can I go back to work after hair transplant?
Desk-based work: 4–7 days. Public-facing or physically demanding work: 10–14 days. The donor and recipient areas show visible redness and small scabs for 7–10 days; most people are back to normal appearance by week 2. A loose-fitting cap can cover the area during the early days if you need to be in public.
When does shock loss start?
Shock loss typically begins around week 3 post-op and continues for 8–12 weeks. By month 3, most original transplanted hair shafts have shed and the follicles are entering or exiting the dormant phase. Regrowth begins around month 3 and accelerates through months 4–6. Full discussion in the shock loss article.
When can I exercise after a hair transplant?
Light walking from day 1. Heart-rate-elevating exercise: avoid for 2 weeks. Gym (cardio + resistance): typically resume from week 3–4. Contact sports (rugby, martial arts): avoid for 6 weeks minimum. Swimming in chlorinated pools: from week 4. Sea/saltwater swimming: from week 5–6. The point of waiting is to avoid head injury during early healing and to prevent excessive scalp blood flow that could displace early grafts.
When can I drink alcohol after a hair transplant?
Avoid alcohol entirely for the first 7 days — it interferes with healing, increases scalp blood flow, and interacts with prescribed medications. Resume in moderation from week 2 onward. Heavy drinking is best avoided through month 1 to support recovery and avoid disrupting the new graft establishment phase.
When are hair transplant results final?
Month 12 is the standard assessment point at which surgical outcome can be honestly evaluated. A small portion of additional density develops between month 12 and month 18 (NHS cosmetic-surgery formal review point), but the difference is modest. Surgeons who recommend touch-up procedures typically do so based on month 9–12 assessment.
When can I fly after a hair transplant?
Most clinics clear flying from day 4 onward. Travel patients booked through Istanbul usually schedule the return flight on day 4 or later so the day-2 wash, day-3 review and at least one supervised home wash happen before departure. A loose hat (not pressing on the recipient area) is fine during the flight; cabin pressure is not a problem.
Is it normal to have swelling on my forehead?
Mild forehead swelling is very common, peaking around day 2–3 and resolving by day 5–7. It’s caused by anaesthetic and fluid shift down to the forehead under gravity. An ice pack on the forehead (not on the recipient area) and sleeping semi-upright reduce it. Severe swelling beyond what’s been described in your clinic’s pre-op information warrants a call.
Will I lose my native hair after a transplant?
Some patients experience native shock loss — temporary shedding of native hair around the transplanted area, caused by surgical trauma. This typically regrows within 3–6 months. The longer-term concern is AGA progression in the surrounding native hair, which is unrelated to the surgery itself and is why most surgeons recommend continuing finasteride and/or minoxidil after transplant to protect native densitynice-mpb.
Sources
- NHS — Hair transplant overview and recovery. https://www.nhs.uk/conditions/cosmetic-procedures/hair-transplant/ ↩
- StatPearls — Hair Transplantation. National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK547740/ ↩
- Sharma R, Ranjan A. “Follicular Unit Extraction (FUE) Hair Transplant: Curves Ahead.” J Med Life. 2019. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6795649/ ↩
- Garg AK et al. “Complications in hair transplantation.” J Cutan Aesthet Surg. 2021. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8719980/ ↩
- International Society of Hair Restoration Surgery — 2024 Practice Census and member directory. https://www.ishrs.org/ ↩
- General Medical Council — The Medical Register. https://www.gmc-uk.org/registration-and-licensing/the-medical-register ↩
- NICE Clinical Knowledge Summary — Male pattern baldness. https://cks.nice.org.uk/topics/male-pattern-baldness/ ↩
Как BergemHealth подходит к этому
Операции выполняются в Liv Hospital Ulus (Стамбул) с аккредитацией JCI доктором Hamid Aydın и резидентной хирургической командой. Консультация в Великобритании и 12-месячный уход в нашем офисе на Harley Street с регулированием CQC. Прозрачные цены и бесплатная корректировка при необходимости.
Бесплатная консультация →