Shock Loss After Hair Transplant: Why It Happens, When It Ends
Shock loss explained: why transplanted hairs shed weeks after surgery, when they regrow, and the asymmetric outcome between transplanted and native hair.
Medical disclaimer. This article is educational and not medical advice. Hair restoration outcomes are individual; only a qualified surgeon can assess your case in a personal consultation.
Quick answer
Shock loss is the temporary shedding of transplanted hair shafts that begins around week 3 post-op and runs through month 3. It is not the surgery failing — the transplanted follicles are alive and anchored; they have temporarily entered the telogen (resting) phase. New growth begins around month 3 and reaches full final density by month 12. The asymmetric outcome to understand: transplanted hairs almost always return because the donor follicle is DHT-resistant, but native hairs in surrounding zones with active androgenetic alopecia may not regrow if surgical trauma triggers shedding of follicles already miniaturisingnice-mpb. This article covers the mechanism, the timeline, and when anxiety is warranted.
Table of contents
- What shock loss actually is
- The mechanism: why follicles enter dormancy
- The timeline: when shock loss starts and ends
- Transplanted hairs vs native hairs (the asymmetric outcome)
- When to wait vs when to call the clinic
- Can shock loss be reduced?
- How BergemHealth handles shock-loss anxiety
- What to do next
- Frequently asked questions
What shock loss actually is
Definition. Shock loss (telogen effluvium induced by surgical trauma) is the temporary shedding of hair shafts in and around the surgical area, starting roughly 2–4 weeks after a hair transplant. Follicles remain intact and viable in the scalp; the hair shaft has shed because the follicle has shifted into its resting phase. New hair grows from the same follicle when the resting phase ends.
Shedding a hair shaft is not the same as losing a follicle. The follicle is the hair-producing organ embedded in the scalp; the shaft is the visible hair. Shock loss sheds shafts. The follicles, in nearly all transplanted cases, remain intact and grow new shafts laterstatpearls. The visible appearance at month 1 may be roughly the pre-surgery picture, but the follicles underneath will produce new hair shafts in a few months.
The mechanism: why follicles enter dormancy
The hair growth cycle has three phases: anagen (active growth, 2–7 years), catagen (transitional, 2–3 weeks), and telogen (resting, 2–4 months). In normal hair, follicles cycle asynchronously — roughly 85–95% are in anagen and 5–15% in telogen at any moment.
Hair transplant extraction and re-implantation is significant trauma at the cellular level. Each follicle is removed from its original blood supply, kept in holding solution, then placed where it must establish fresh vasculature. The biological response is to shift many affected follicles synchronously into telogen — they enter the resting phase together, hold their shafts loosely for 2–4 weeks, then shed those shafts together. The follicles re-enter anagen on their normal cycle timing once they’ve established new vasculature. By month 3, most have begun producing new hair shafts; by month 6–12, those new shafts have grown to mature length and thicknesssharma.
The timeline: when shock loss starts and ends
The typical timeline for transplanted-hair shock loss:
| Timeframe | What’s happening |
|---|---|
| Week 0–2 | Transplanted hair shafts visible as short stubble; follicles still in anagen from before extraction |
| Week 2–4 | Many follicles synchronously enter catagen; shafts begin loosening |
| Week 4–8 | Peak shedding period; transplanted hair shafts release with normal washing or gentle handling |
| Week 8–12 | Most original shafts have shed; follicles are in deep telogen |
| Week 12–16 (Month 3) | New growth begins from many follicles; thin, fine, often colourless hairs emerge |
| Month 3–6 | Progressive thickening and lengthening of new shafts |
| Month 6–12 | Full density emerges (50% by month 6, 90%+ by month 12) |
Different follicles enter and exit telogen at slightly different times, which is why regrowth doesn’t happen all at once. A portion of native hair around the transplant zones may also undergo shock loss; this typically resolves on the same 3–6 month timeline — with the important caveat covered in the next section.
For the explicit milestone-by-milestone visible appearance, see the month-by-month results article.
Transplanted hairs vs native hairs (the asymmetric outcome)
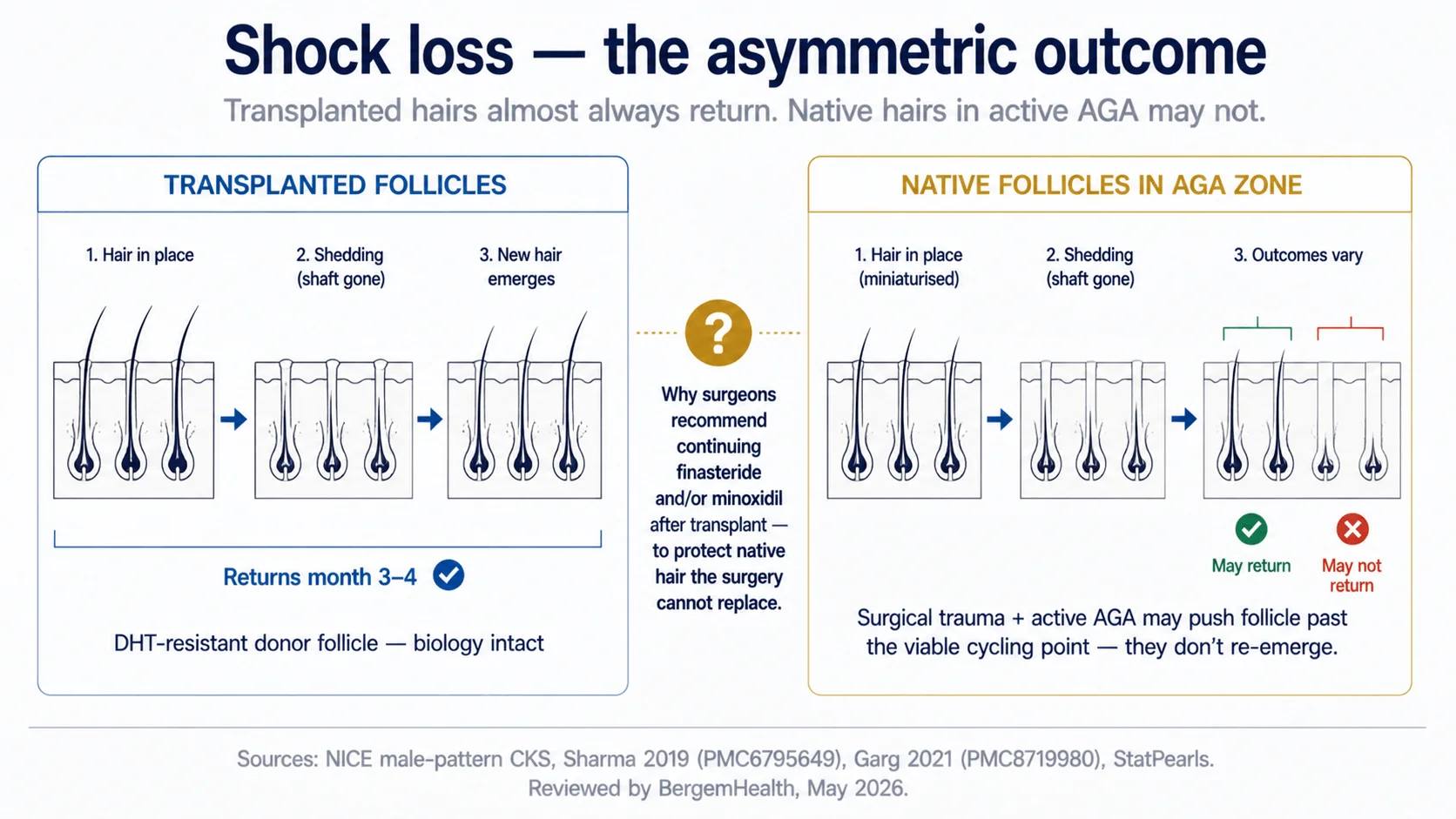
Definition. Asymmetric outcome refers to the different long-term prognosis of transplanted versus native hairs after the surgical procedure. Transplanted follicles, having come from the DHT-resistant donor zone, almost always return to full growth after shock loss. Native follicles in the surrounding AGA-affected zones can return to growth, fail to return, or return temporarily and then resume their previous miniaturisation trajectory.
This is the part of shock loss that most patient resources skip or minimise. The honest version:
Transplanted hair shock loss is reversible in nearly all cases. The follicles are biologically unchanged by the move — they retained their DHT-resistance during extraction, re-establish blood supply in the new location, and resume normal anagen-catagen-telogen cycling, producing donor-zone-quality hair indefinitely.
Native hair shock loss is more variable. Surgical trauma in the recipient area affects the patient’s existing native follicles in the same zone. If those native follicles were healthy, they recover and resume normal cycling. If they were already in active AGA and approaching the end of their viable cycling — which is often the case in the recipient zone, by definition — surgical trauma can push them past the point of return. They enter telogen and may not re-emergenice-mpb.
What this means in practice: at month 6, density looks lower than hoped because some regained transplanted density is offset by native hair that didn’t recover. At month 12, density looks closer to expectation. By year 2–3, density may further reduce in surrounding native zones if AGA continues to progress — which is why most surgeons recommend continuing finasteride and/or minoxidil after transplant (see the AGA article and the hair treatment pillar).
This isn’t a reason not to have surgery — it’s a reason to have realistic expectations about what the surgery does (restores density at affected zones) and what it doesn’t do (change the underlying AGA process).
When to wait vs when to call the clinic
| Symptom | Normal? | Action |
|---|---|---|
| Hair shafts shedding weeks 3–10 | Yes | Wait; this is shock loss |
| Recipient looking “back to pre-surgery” weeks 8–12 | Yes | Wait; this is the lowest point |
| Some native hair shedding around the transplant area | Yes | Wait; usually recovers in 3–6 months |
| Patchy shedding weeks 4–10 | Yes | Wait; follicles cycle asynchronously |
| Donor-area shock loss (small bald patches at back/sides) | Sometimes | Photograph and contact clinic — usually resolves |
| No new growth at month 4 | Probably normal but worth checking | Clinic review; trichoscopy confirms follicles are present |
| No new growth at month 6 | Concerning | Contact clinic — past typical regrowth onset |
| Sudden new bald patch months later | Not normal | Contact clinic; possible alopecia areata |
| Inflammation, redness, scaling weeks/months later | Not normal | Contact clinic; possible folliculitis |
If month 4 has come and gone without any new growth, a clinical review with trichoscopy is the right next step. The published complication-rate literature reports serious adverse events at well under 1%garg.
Can shock loss be reduced?
The biological process of follicles entering telogen after surgical trauma is largely unavoidable — it’s the body’s normal response. Three variables affect it modestly:
- Surgical technique: meticulous handling of grafts during extraction and implantation reduces the proportion of follicles shocked into telogen. This is one of the variables that distinguishes surgeon-led from technician-led practice (see red flags).
- Pre-op finasteride and minoxidil: most surgeons recommend continuing existing therapy through surgery and into recovery, both to protect native hair and to support follicle health.
- Post-op care discipline: avoiding alcohol in week 1, smoking, heavy exercise too early and scratching at crusts reduces compounding stressors.
What does not meaningfully reduce shock loss: shampoos marketed as “post-transplant”, supplements without a deficiency present, scalp massages early in recovery, or “shock loss prevention” protocols without evidence base. Shock loss is mostly biology, not technique-dependent at the patient level.
How BergemHealth handles shock-loss anxiety
Shock-loss anxiety is the most common reason patients message the aftercare team between scheduled reviews. The standard response: photograph the recipient area in identical lighting to the day-7 photo, send it to the clinic, get a same-day assessment. Structured reviews at month 1, 3, 6, 9, and 12 are part of the 12-month aftercare bundle included at both Liv Hospital Ulus and 99 Harley Street.
Dr. Hamid Aydın leads the surgical pathway at Liv Hospital Ulus (ISHRS member, 25,000+ procedures since 2000)ishrs; Dr. Sumeyye Yuksel leads the London consulting and aftercare teamgmc.
What to do next
For the broader 12-month timeline, see the recovery-aftercare pillar. For the day-by-day picture of weeks 1–2, see first 7 days after FUE. For the milestones at month 1 / 3 / 6 / 9 / 12, month-by-month results. For the biology of why native hair may not always recover, see androgenetic alopecia. For the methods themselves, see the hair-transplant pillar.
If you’re in the post-op shock-loss phase and the photos are causing anxiety, request a free assessment from BergemHealth’s London or Istanbul team — even if your surgery was elsewhere. A second-opinion review with trichoscopy can confirm whether your timeline is normal.
Frequently asked questions
Is shock loss normal after hair transplant?
Yes — it’s expected and biologically normal. Transplanted follicles enter the telogen phase synchronously after surgical trauma; visible hair shafts shed; new shafts grow from the same follicles around month 3. Most patients reach 50% of final density by month 6 and 90%+ by month 12.
When does shock loss happen?
Shedding typically begins 2–4 weeks post-op, peaks at weeks 4–8, and substantially completes by week 10–12. New growth begins around month 3.
Do all transplanted hairs fall out?
Most do, but not all. Some transplanted hairs continue growing without shedding — these are follicles that didn’t enter telogen synchronously. The proportion varies and isn’t predictable. Either pattern is normal.
When do transplanted hairs grow back?
New growth begins around month 3, accelerates through months 4–6, and continues to thicken through months 6–12. Month 12 is the standard assessment point.
Will my native hair grow back after shock loss?
Usually yes, with caveats. Healthy native follicles recover and resume normal cycling. Native follicles in surrounding zones already in active AGA and approaching the end of viable cycling may not returnnice-mpb — this is the asymmetric outcome covered above, and the reason most surgeons recommend continuing finasteride and/or minoxidil after transplant.
How long does shock loss last?
Shedding phase: roughly 4–8 weeks (weeks 3–10 post-op). Dormancy before new growth: until month 3. Full recovery to mature density: month 12. The visible phase lasts about 8–10 weeks; the consequences resolve over 12 months.
Can shock loss be prevented?
The biological process is largely unavoidable. Surgical technique reduces the proportion of follicles affected; pre-op finasteride and minoxidil protect native hair; post-op care reduces compounding stressors. No protocol eliminates shock loss entirely.
What if no new hair has grown by month 4?
Schedule a clinic review. Most patients have early new growth by month 4. No visible growth at month 4 isn’t necessarily a problem — follicles can remain in extended telogen — but trichoscopy confirms follicles are present and healthy. By month 6, lack of new growth is more concerning.
Sources
- StatPearls — Hair Transplantation. National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK547740/ ↩
- Sharma R, Ranjan A. “Follicular Unit Extraction (FUE) Hair Transplant: Curves Ahead.” J Med Life. 2019. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6795649/ ↩
- Garg AK et al. “Complications in hair transplantation.” J Cutan Aesthet Surg. 2021. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8719980/ ↩
- NICE Clinical Knowledge Summary — Male pattern baldness. https://cks.nice.org.uk/topics/male-pattern-baldness/ ↩
- International Society of Hair Restoration Surgery — Member directory. https://www.ishrs.org/ ↩
- General Medical Council — The Medical Register. https://www.gmc-uk.org/registration-and-licensing/the-medical-register ↩
How BergemHealth approaches this
Procedures are performed at JCI-accredited Liv Hospital Ulus, Istanbul, by Dr. Hamid Aydın and the resident surgical team. UK consultation and 12-month aftercare at our CQC-regulated Harley Street office. Transparent pricing and a free touch-up if indicated.
Free consultation →