Androgenetic Alopecia (Male Pattern Baldness): Full Guide 2026
Androgenetic alopecia explained: how DHT miniaturises follicles, how to tell AGA from lookalikes, the DUPA exception, and what actually treats it.
Medical disclaimer. This article is educational and not medical advice. Hair restoration outcomes are individual; only a qualified clinician can assess your case in a personal consultation.
Quick answer
Androgenetic alopecia (AGA) is genetic, hormone-mediated hair loss in which scalp follicles in susceptible regions are progressively miniaturised under the influence of dihydrotestosterone (DHT). It’s the most common form of hair loss in men — affecting roughly 50% by age 50 — and the form best suited to combined medical management and hair transplant. The diagnostic challenge isn’t recognising AGA; it’s distinguishing it from lookalikes — post-viral telogen effluvium, iron-deficiency shedding, and the rarer diffuse unpatterned alopecia (DUPA) where the “donor zone” assumption breaks down. This article walks through the mechanism, pattern, lookalikes, and treatments that actually work.
Table of contents
- What androgenetic alopecia actually is
- The mechanism: DHT, follicle miniaturisation, and genetics
- Who gets it, when, and how fast
- The pattern (and how it differs from female pattern hair loss)
- Distinguishing AGA from its lookalikes
- The DUPA exception: when the donor zone isn’t safe
- Treatment options for AGA
- How BergemHealth approaches AGA
- What to do next
- Frequently asked questions
What androgenetic alopecia actually is
Definition. Androgenetic alopecia is a genetically-determined sensitivity of certain scalp hair follicles to androgens — specifically dihydrotestosterone — that causes those follicles to undergo progressive miniaturisation across successive hair-growth cycles. The follicles produce shorter, thinner, less-pigmented hairs at each cycle until eventually they produce only vellus hair or stop producing hair altogether.
Three points follow from that definition:
- AGA is not a single bad event — it’s a slow shift across many hair cycles. The hairs are still there in early stages; they’re just getting thinner and shorter.
- AGA is region-specific. It affects follicles in the frontal and crown areas because those follicles are genetically programmed to be androgen-sensitive. The follicles at the back and sides — the donor zone — typically aren’t, which is the biological basis of hair transplantation.
- AGA is progressive. Untreated, it tends to continue. A 28-year-old at Norwood II is rarely “stable”; the trajectory is decadal.
NICE Clinical Knowledge Summaries describe AGA as the most common cause of hair loss in men and women, with a strong genetic component and clear response to androgen-suppressing therapy in mennice-mpb.
The mechanism: DHT, follicle miniaturisation, and genetics
The molecular story has three components:
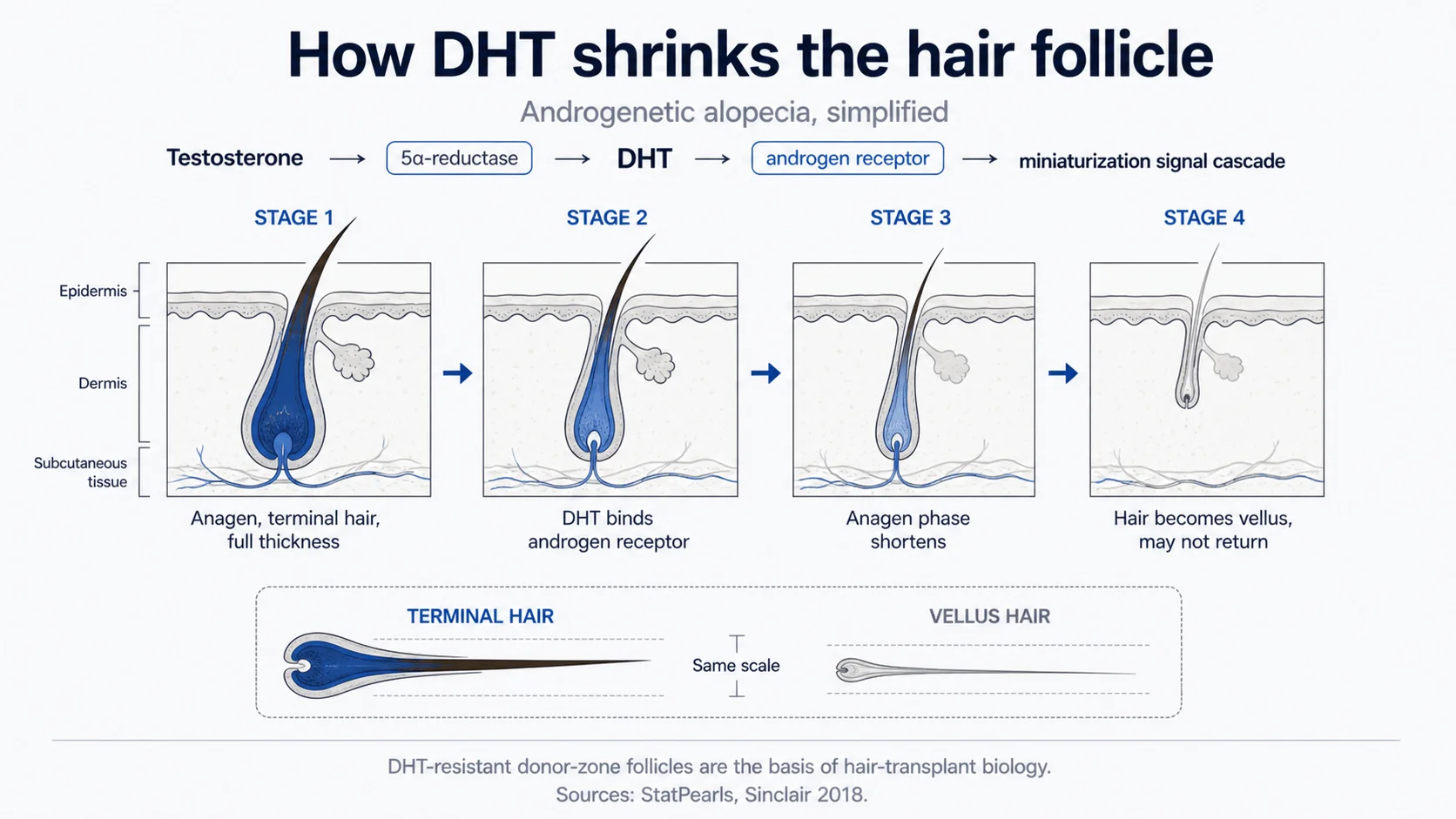
1. Testosterone → DHT conversion. The enzyme 5-alpha-reductase converts testosterone to its more potent form, dihydrotestosterone. DHT is the active androgen at the hair follicle level.
2. The androgen receptor (AR) at the follicle. Hair follicles in AGA-susceptible regions express androgen receptors. When DHT binds, it triggers a signalling cascade that shortens the follicle’s anagen (growth) phase, increases time spent in telogen, and reduces the size of the hair shaft producedstatpearls.
3. Genetic susceptibility. Whether a follicle is AGA-susceptible is genetically determined. The androgen receptor gene is on the X chromosome (which men inherit from their mothers) and variants of this gene are the most strongly associated risk factor — but it’s not single-gene; multiple loci contribute, which is why family-history correlation is real but imperfect.
The treatment implication: reduce DHT (finasteride) or extend the anagen phase (minoxidil) and you slow or partially reverse miniaturisation at the susceptible follicles. Donor follicles aren’t AR-sensitive, so they keep growing normally — which is why transplanted hair retains its growth pattern in the recipient zone.
Who gets it, when, and how fast
The epidemiological picture in men of European ancestry:
- By age 30: roughly 25–30% show some AGA patternnice-mpb
- By age 50: roughly 50%
- By age 70: 70–80% lifetime prevalence
Prevalence is somewhat lower in men of African ancestry, lower still and later-onset in men of East Asian ancestry. Roughly 16% of men aged 18–29 already show Norwood II–III recessionnice-mpb.
Pace of progression is the variable patients most want predicted, and the hardest to predict reliably. Some men progress from Norwood II to V over 5 years; others stay at Norwood III for 20. Initial pace doesn’t strongly predict eventual stage. Variables that do predict faster progression: earlier age of onset, strong family history of advanced AGA on either side, and high baseline DHT sensitivity (inferred from clinical pattern, not routinely measured).
The pattern (and how it differs from female pattern hair loss)
Male AGA follows recognisable patterns that the Norwood scale classifies into 7 main stages plus a Type A variant. Classic features:
- Bitemporal recession (the temple corners receding upward and back)
- Vertex (crown) thinning, sometimes preceding frontal recession
- A “bridge” of hair between front and crown that narrows in advanced cases
- Preserved donor zone at the back and sides
Female pattern hair loss (FPHL) typically presents differently:
- Diffuse central thinning with widening of the parting (the “Christmas tree” pattern from above)
- Frontal hairline preserved — total frontal recession in a woman warrants consideration of frontal fibrosing alopecia or another diagnosis
- Sides and back also affected in some women, making donor area assessment more careful
Female AGA is often classified by the Ludwig scale (Types I–III)ludwig, covered in the main Hair Loss pillar. Both sexes can have AGA; the biological mechanism is similar, but treatment options differ — finasteride is contraindicated in women of childbearing age.
Distinguishing AGA from its lookalikes
Three conditions get repeatedly confused with AGA in the early stages, and the treatments differ.
Lookalike 1: Telogen effluvium (TE). TE is temporary shedding triggered by an event 2–3 months earlier (illness, surgery, childbirth, severe stress, weight loss). The shedding is diffuse — including the sides and back of the scalp — whereas AGA is patterned (frontal and crown). TE hairs on the pillow have normal shaft thickness; AGA hairs are miniaturised and thinner. TE resolves spontaneously over 6–12 months once the trigger is identified; AGA progresses without treatment. Post-COVID shedding is the most common TE in 2024–2026 and is frequently misdiagnosed as accelerating AGA — a 30-minute trichoscopy consultation distinguishes them.
Lookalike 2: Iron deficiency or thyroid-related shedding. Low ferritin (even when haemoglobin is normal), hypothyroidism, and hyperthyroidism can all produce diffuse hair shedding. The clue: the shedding is diffuse, the blood test is abnormal, and the hair recovers fully when the underlying issue is treated. Standard NHS panels (FBC, ferritin, TSH, vitamin D) catch most of thesenhs.
Lookalike 3: Drug-induced shedding. Multiple medications can cause hair shedding — beta-blockers, statins, anticonvulsants, oral retinoids, lithium, some antidepressants. The pattern is diffuse, starts within months of beginning the drug, and resolves within 6 months of stopping it. If your hair loss began within a year of a new medication, ask your GP.
The diagnostic shorthand: AGA is patterned and progressive; the lookalikes are diffuse and resolvable. Trichoscopy distinguishes them when in doubttrichology.
The DUPA exception: when the donor zone isn’t safe
Most AGA patients have a DHT-resistant donor zone. A small but important minority have diffuse unpatterned alopecia (DUPA) — a variant in which the entire scalp, including the back and sides, is androgen-sensitive. In DUPA, the donor zone miniaturises along with the rest of the scalp, just at a slower rate.
DUPA matters because DUPA patients are not good hair-transplant candidates. Transplanted follicles, having come from an AGA-susceptible donor zone, will eventually miniaturise in the recipient area too — defeating the purpose of the transplant. Standard surgical practice treats DUPA as a contraindication, or at minimum a strong cautionary signalstatpearls.
DUPA is identified by:
- Diffuse miniaturisation visible on trichoscopy across the entire scalp, including occipital and lateral regions
- Reduced donor density on direct examination
- Family history of advanced diffuse hair loss without classic Norwood patterning
- Age-of-onset sometimes earlier than typical AGA
A clinic that doesn’t examine the donor zone in detail before quoting a transplant is skipping the most important pre-op variable. (See what to ask before booking.)
Treatment options for AGA
The treatment pyramid for confirmed AGA in 2026:
| Tier | Intervention | Evidence | Realistic effect |
|---|---|---|---|
| Tier 1 (drugs) | Finasteride (oral 1mg) | Meta-analysis supportmella-fin | Stabilisation in ~80–90% of men; modest density gain |
| Tier 1 (drugs) | Minoxidil topical (5%) or low-dose oral | Cochrane support for topicalcochrane-min; growing evidence for oralsinclairvano | Modest density gain; synergistic with finasteride |
| Tier 2 (procedures) | PRP, mesotherapy, LLLT | Mixed RCTs, more variable | Adjunct to Tier 1; not transplant replacements |
| Tier 3 (surgery) | Hair transplant (FUE, Sapphire FUE, Direct DHI) | Surgical literaturestatpearls | Restores density to recipient zone; doesn’t change AGA process in surrounding hair |
A realistic 2026 plan for a man newly diagnosed at Norwood II–III: start finasteride 1mg daily (full side-effect discussion in the finasteride article); add minoxidil topical 5% twice daily or low-dose oral if specialist-prescribed (the minoxidil article); review at 12 months with photographs and trichoscopy; continue indefinitely (AGA returns within 6–12 months of stopping); reassess for transplant at 12–24 months if visible loss has progressed beyond what medical management stabilises.
A man already at Norwood IV–V at first presentation gets the same medical management layered with an earlier hair-transplant decision, because medical management alone usually can’t restore lost density at advanced stages. The combined approach — medical management to protect native hair, plus transplant to restore density — is what most surgeons consider best practice for moderate-to-advanced AGA. The hair transplant pillar covers method choice; FUE vs DHI vs Sapphire walks through which method suits which case.
The main risk is not starting treatment early enough — every year of untreated AGA is a year of additional miniaturisation that won’t be reversed.
How BergemHealth approaches AGA
BergemHealth’s first-consultation pathway treats AGA the same whether the patient walks into Harley Street in London or Liv Hospital Ulus in Istanbul: clinical history, trichoscopy of frontal and donor regions, donor-density measurement, and a discussion of which treatment tier is appropriate at the patient’s current stage.
For early-stage AGA (Norwood II–III), the recommendation is usually medical management first — the finasteride and minoxidil decisions get the same evidence-based discussion they would in a UK private dermatology consultation. For moderate-to-advanced AGA (Norwood IV+), the conversation expands to include surgical planning, with medical management continuing alongside.
The DUPA assessment is built into every donor-area examination because it changes the recommendation entirely. Roughly 1 in 30 men presenting for hair-transplant assessment have features warranting a “no, transplant isn’t appropriate” answer — and giving that answer honestly is part of the assessment.
Per-graft pricing is the same on both sides of the network: from £1,250 (Standard FUE), £1,750 (Sapphire FUE), £2,250 (Direct DHI). Surgery — when indicated — happens at Liv Hospital Ulus (Istanbul, JCI-accredited) or 99 Harley Street (London, CQC-registered); the choice between locations is logistical. Dr. Sumeyye Yuksel leads the GMC-registered consulting team at Harley Streetgmc; the surgical pathway in Istanbul is led by Dr. Hamid Aydın (ISHRS, 25,000+ procedures since 2000)ishrs.
What to do next
If your hair loss looks like AGA at an early stage, start medical management — see the finasteride article and the minoxidil article, or speak to your GP. PRP can be considered as an adjunct (detail here).
If your AGA looks moderate-to-advanced, request a free assessment from BergemHealth’s London or Istanbul team. The consultation includes trichoscopy, donor-area assessment with DUPA screening, graft-count estimate where surgery is appropriate, and an honest answer about whether the timing is right.
For staging help, see the Norwood walkthrough; for younger patients deciding whether early changes are AGA or normal maturation, see the early-signs guide. For broader diagnostic context, see the Hair Loss pillar.
Frequently asked questions
At what age does male pattern baldness start?
AGA can begin in the late teens; first identifiable patterning is most common in the 20s and 30s. Roughly 16% of men aged 18–29 already show Norwood II–III recessionnice-mpb. Earlier onset typically predicts more advanced eventual stage, though pace varies widely.
Can I stop AGA from getting worse without taking finasteride?
Topical minoxidil 5% has Cochrane-level evidence for slowing AGA progression and producing modest density gains without affecting DHT — a reasonable monotherapy option for men who can’t or won’t take finasteridecochrane-min. The effect is smaller than finasteride plus minoxidil, but it’s real. PRP and LLLT are sometimes added as adjuncts.
Is DHT the only hormone involved in AGA?
DHT is the dominant androgen in AGA pathophysiology and the one targeted by finasteride. Other hormones — testosterone, DHEA, oestrogens — interact with the system, but DHT and the androgen receptor are the central playersstatpearls. Hormonal investigations beyond standard panels are rarely indicated in routine male AGA.
How do I know if I have DUPA?
DUPA is identified by trichoscopy showing miniaturisation across the entire scalp including back and sides, plus reduced donor density on direct measurement. It’s diagnosed by a clinician with a dermatoscope, not by self-assessment. If you’re considering hair transplant, the donor area examination should specifically screen for DUPA features.
Will finasteride stop my hair loss long-term?
Finasteride stabilises AGA progression in roughly 80–90% of men who take it, and produces modest density gains in manymella-fin. The effect persists as long as the drug is taken; AGA progression typically resumes within 6–12 months of stopping treatment. So finasteride is a long-term therapy, like a statin for cholesterol, not a one-off cure. Detailed side-effect discussion in the finasteride article.
Does masturbation, gym training, or testosterone level affect AGA?
No. AGA is driven by genetic sensitivity of follicles to DHT at normal physiological levels. Variations in serum testosterone within the normal range don’t strongly affect AGA. Masturbation has no clinically meaningful effect. Gym training raises testosterone modestly and transiently but doesn’t accelerate AGA. Anabolic steroid use is different — supraphysiological androgens can accelerate AGA in susceptible men.
Can AGA be reversed?
Partial reversal — recovery of some follicle size and density — is possible at earlier stages with finasteride and minoxidil, particularly when treatment starts before substantial miniaturisation. Complete reversal of fully miniaturised follicles is generally not possible. Hair transplant addresses density loss at affected zones but doesn’t change the AGA process in surrounding follicles.
Is there a blood test that confirms AGA?
No single blood test confirms AGA. The diagnosis is clinical, based on pattern, distribution, family history, and trichoscopy. Blood tests rule out lookalikes — FBC, ferritin, TSH, vitamin Dnhs. Commercial genetic testing for AGA susceptibility rarely changes management.
Why does my hair shed seasonally?
Mild seasonal shedding is recognised — many people shed slightly more in late summer and autumn. It’s not AGA. The shed should be mild and self-limiting (resolving within 1–2 months). Heavy seasonal-feeling shedding lasting beyond 3 months is more likely telogen effluvium with a different trigger and warrants clinical review.
Sources
- NHS — Hair loss overview. https://www.nhs.uk/conditions/hair-loss/ ↩
- NICE Clinical Knowledge Summary — Male pattern baldness. https://cks.nice.org.uk/topics/male-pattern-baldness/ ↩
- StatPearls — Androgenetic Alopecia. National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK430924/ ↩
- Mella JM et al. “Efficacy and safety of finasteride therapy for androgenetic alopecia.” Arch Dermatol. 2010. DOI: 10.1001/archdermatol.2010.256 ↩
- Gupta AK, Charrette A. “Topical minoxidil for androgenetic alopecia.” Cochrane Database Syst Rev. DOI: 10.1002/14651858.CD007628 ↩
- Sinclair RD. “Female pattern hair loss: combination therapy with low-dose oral minoxidil.” Int J Dermatol. 2018. DOI: 10.1111/ijd.13838 ↩
- Vañó-Galván S et al. “Safety of low-dose oral minoxidil for hair loss.” J Am Acad Dermatol. 2021. DOI: 10.1016/j.jaad.2020.06.1023 ↩
- Ludwig E. “Classification of the types of androgenetic alopecia (common baldness) occurring in the female sex.” Br J Dermatol. 1977. DOI: 10.1111/j.1365-2133.1977.tb15179.x ↩
- Institute of Trichologists (UK) — Position statements. https://www.trichologists.org.uk/ ↩
- International Society of Hair Restoration Surgery — 2024 Practice Census and member directory. https://www.ishrs.org/ ↩
- General Medical Council — The Medical Register. https://www.gmc-uk.org/registration-and-licensing/the-medical-register ↩
How BergemHealth approaches this
Procedures are performed at JCI-accredited Liv Hospital Ulus, Istanbul, by Dr. Hamid Aydın and the resident surgical team. UK consultation and 12-month aftercare at our CQC-regulated Harley Street office. Transparent pricing and a free touch-up if indicated.
Free consultation →