Norwood Scale Explained: Hair Loss Stages 1 to 7 (Visual Guide)
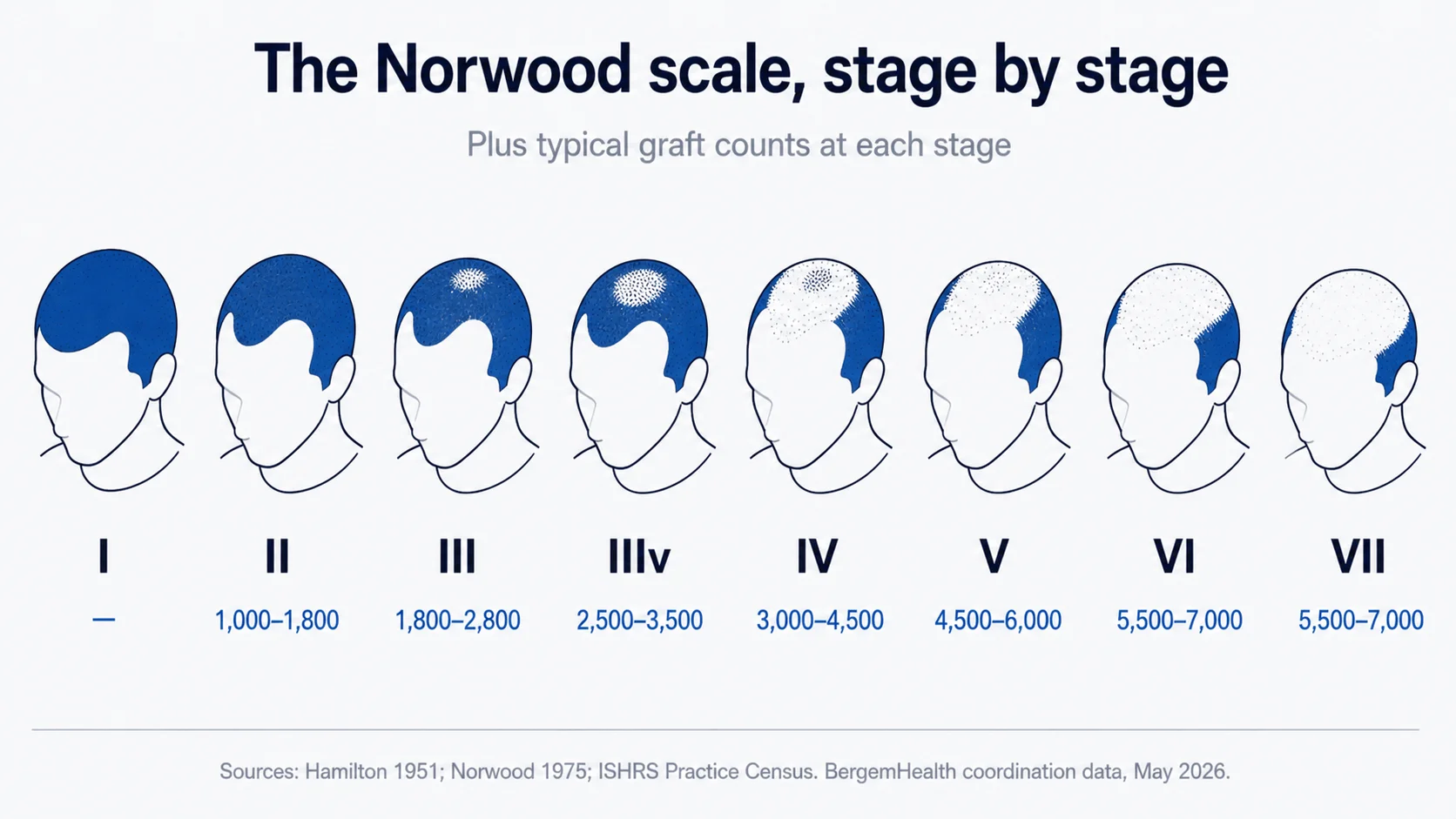
The Norwood scale stage-by-stage: I to VII plus Type A and IIIv variants, with typical graft counts at each stage and how the scale guides treatment decisions.
Medical disclaimer. This article is educational and not medical advice. Hair restoration outcomes are individual; only a qualified clinician can assess your case in a personal consultation.
Quick answer
The Norwood-Hamilton scale (1975) is the standard staging system for male androgenetic alopecia, with seven main stages plus the Type A and IIIv variants. Stage maps directly onto treatment decisions and graft requirements: II–III is usually managed medically first; IV–V is the typical hair-transplant candidate stage; VI–VII often needs staged surgery and careful donor planning. This guide walks each stage in plain English, with realistic graft-count ranges.
Table of contents
- What the Norwood scale is
- The seven main stages, walked through
- The Type A variant (the often-skipped one)
- The IIIv vertex variant
- Typical graft count by Norwood stage
- Why staging guides treatment, not just describes it
- Limits of the Norwood scale
- How BergemHealth uses staging
- What to do next
- Frequently asked questions
What the Norwood scale is
Definition. The Norwood-Hamilton scale is a visual classification system for male androgenetic alopecia (AGA), originally proposed by James Hamilton in 1951 and modified by O’Tar Norwood in 1975. It identifies seven main stages of pattern hair loss based on frontal hairline and vertex (crown) appearance, plus the Type A and IIIv variantsnorwood.
Why the scale matters: it’s the lingua franca between patient, GP, dermatologist, trichologist, and surgeon — “Norwood IV” means roughly the same thing to all of them. It maps onto graft-count expectations and medical-management decisions, and lets year-over-year photos be staged consistently.
The scale is for men. The female equivalent is the Ludwig scale, covered in the main Hair Loss pillar.
The seven main stages, walked through
Norwood I — no visible recession. Adolescent hairline, even and rounded. The baseline.
Norwood II — slight temporal recession. Mild recession at the temples; the hairline has a slight backward angle at the corners. Caveat: small bitemporal recession is part of normal adult hairline maturation in many men. The distinction (covered in the early-signs guide) depends on whether the recession is symmetric and stable (maturing hairline) or progressive with miniaturisation (early AGA).
Norwood III — recognisable temporal recession. Recession clearly deeper at the corners, forming the M-shape or U-shape. Vertex typically still intact at III, though thinning may be beginning. Usually the earliest stage at which men start to notice pattern hair loss.
Norwood IV — pronounced recession with vertex thinning. Frontal hairline has receded significantly; vertex shows visible thinning. A bridge of hair still separates front from crown — two distinct areas of loss.
Norwood V — narrowing bridge. The bridge between front and crown is thinning. The two areas are starting to feel visually connected.
Norwood VI — bridge gone. Frontal and vertex areas have merged into one large area of advanced loss. The donor zone behind and at the sides is preserved.
Norwood VII — extensive baldness. Only a horseshoe of donor hair remains. The top of the scalp is essentially bald.
Most patients move through these stages over years to decades — faster early (I → III over 5–10 years) than late (V → VII can take 15+), with wide individual variability.
The Type A variant (the often-skipped one)
The Norwood scale identifies a Type A pattern that doesn’t follow the standard front-then-crown progression. In Type A, the hairline recedes uniformly front-to-back without a distinct vertex thinning stage — IIA → IIIA → IVA → VA, the loss progressing back across the scalp like a slowly-rising tide rather than as separate frontal and vertex areas.
Why Type A matters: graft-count maths differs (more contiguous area often needs more grafts at “equivalent” stages); the cosmetic presentation lacks the M-shape that’s the cultural shorthand for “balding”, so patients sometimes self-assess as less advanced than they are; surgery’s visible benefit usually requires Type-A-equivalent Norwood IV before it’s meaningful.
Roughly 5–10% of male AGA cases follow Type A. Standard clinical examination identifies it.
The IIIv vertex variant
Norwood IIIv = III recession plus prominent vertex thinning. Standard III has minimal crown involvement; IIIv has significant crown involvement at the same stage. Patients at IIIv have different surgical priorities — the vertex is the cosmetically dominant concern, where standard III patients focus on the hairline.
Typical graft count by Norwood stage
These are ranges — actual counts depend on donor density, hair characteristics (curl, calibre, density per follicular unit), and the cosmetic targets agreed in consultation.
| Norwood stage | Typical graft count | Surgical strategy |
|---|---|---|
| II | Usually not transplanted; medical management | Defer surgery; finasteride/minoxidil first |
| III | 1,500–2,500 | Single session usually sufficient; hairline restoration focus |
| IIIv | 1,800–2,800 | Hairline plus vertex coverage; sometimes staged across two sessions |
| IV | 2,500–3,500 | Single session typically; strategic density distribution |
| V | 3,000–4,000 | Single large session or staged depending on donor quality |
| VI | 4,000+ | Often staged; donor density is the key constraint |
| VII | 4,500+, often 6,000+ | Almost always staged; donor density usually limiting |
Method choice (Standard FUE, Sapphire FUE, Direct DHI) is separate from graft-count planning — covered in the methods comparison.
What constrains graft count at advanced stages is donor density. The donor zone has a finite supply; once extracted, follicles aren’t coming back. At Norwood VI–VII the surgical question shifts from “how many do you need?” to “how many can you safely extract while keeping the donor area cosmetically acceptable?”. This is why advanced cases often need staged surgery.
Why staging guides treatment, not just describes it
Norwood staging changes the clinical recommendation in three concrete ways:
1. Medical management vs surgical planning. At II–III, surgery’s visible benefit is small and the trajectory uncertain — 12–24 months of medical management lets you assess response. At IV+, visible loss is too established for medical management alone to restore lost density, and combined pathways are more useful.
2. Single-session vs staged surgery. III–V are typically single-session candidates. VI–VII often need staged surgery — large graft counts and donor-area economics both demand it.
3. Realistic cosmetic expectations. A Norwood III patient can realistically expect near-complete frontal density restoration. A Norwood VII patient is realistically aiming for strategic redistribution of remaining donor hair to create the impression of density, not a return to pre-AGA appearance.
Limits of the Norwood scale
The scale stages appearance, not the severity of underlying miniaturisation — two patients at “Norwood III” can have very different trichoscopy pictures and prognoses. It doesn’t capture DUPA (covered in the AGA article), doesn’t account for rate of progression (which can vary 5-fold between patients at the same stage), and the boundaries between stages are continuous so two surgeons can reasonably stage the same patient differently by half a stage. Trichoscopy, donor assessment, family history, and progression rate over 12–24 months all matter alongside the stage.
How BergemHealth uses staging
Every BergemHealth pre-surgical assessment includes Norwood staging — but as the starting point, not the conclusion. The discussion that follows looks at trichoscopy, rate of progression, donor density, graft-count range, and whether single-session or staged surgery fits alongside medical management.
Per-graft pricing is the same on both sides: from £1,250 (Standard FUE), £1,750 (Sapphire FUE), £2,250 (Direct DHI). Surgery happens at Liv Hospital Ulus (Istanbul, JCI-accredited) or 99 Harley Street (London, CQC-registered) — the choice is logistical. Dr. Sumeyye Yuksel leads the GMC-registered consulting team at Harley Streetgmc; the surgical pathway in Istanbul is led by Dr. Hamid Aydın (ISHRS, 25,000+ procedures since 2000)ishrs.
What to do next
If you’ve staged yourself and want to understand AGA in depth, see the AGA article. For young patients deciding whether early changes are AGA or normal hairline maturation, the early-signs guide is the right starting point. Broader context: the Hair Loss pillar.
At Norwood II–III, medical management is usually the first step — see the hair treatment pillar.
At Norwood IV+ and considering hair transplant, request a free assessment from BergemHealth’s London or Istanbul team. Method choice is covered in the method comparison.
Frequently asked questions
What Norwood am I?
Look at the seven-stage walkthrough above and find the closest match. Most patients can identify their stage to within half a stage from photographs of the front, top, and crown taken in similar lighting. Clinical assessment refines staging with trichoscopy and progression rate. If you’re between stages — late III or early IV — the difference rarely changes the treatment recommendation.
How fast does AGA progress between Norwood stages?
Highly variable. Some men progress from II to V over 5 years; others stay at III for 20+ years. Earlier age of onset and strong family history correlate with faster progression. Initial pace is a weak predictor. Photographs every 12 months are the most reliable way to track your own rate.
Can I skip Norwood stages?
In a sense, yes — the stages are discrete labels on a continuous spectrum. A patient can present for the first time at Norwood V because earlier stages happened gradually and weren’t seen by a clinician. The biological progression is always gradual.
What’s the difference between Norwood 5 and 6?
The bridge of hair between the frontal recession and the vertex thinning. At V the bridge is narrow but visibly present; at VI it has disappeared and the two areas have merged into one continuous bald area. The transition often coincides with significant changes to surgical planning — VI usually needs more grafts and more careful donor-area management.
Is Norwood 7 transplantable?
Sometimes, with caveats. The constraint is donor density — extracting too aggressively from the remaining horseshoe produces visible thinning. Realistic VII plans aim for strategic density redistribution (creating the impression of coverage at the front) rather than a full return to pre-AGA appearance. Some VII patients aren’t surgical candidates because donor density is too low.
How do I know if I have a Type A pattern?
Type A patterns recede uniformly back across the top of the scalp without a distinct vertex thinning stage. About 5–10% of male AGA cases follow this pattern. Confirmation needs clinical examination — the medical and surgical decisions are essentially the same, with adjusted graft-count expectations.
Can finasteride or minoxidil reverse Norwood stages?
Partial reversal is possible at earlier stages, particularly when treatment starts before substantial miniaturisationmella-fincochrane-min. Complete reversal of fully miniaturised follicles isn’t generally possible. Practically: at II–III, medical management can sometimes shift visible appearance back toward I–II; at V+, it primarily prevents further progression.
Is Norwood staging used for women?
No — women use the Ludwig scale (Types I–III)ludwig, which stages female pattern hair loss based on diffuse central thinning rather than frontal-and-vertex pattern. The biological mechanism is similar in women; the pattern differs and the staging reflects that.
Sources
- Norwood OT. “Male pattern baldness: classification and incidence.” South Med J. 1975. ↩
- StatPearls — Androgenetic Alopecia. National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK430924/ ↩
- NICE Clinical Knowledge Summary — Male pattern baldness. https://cks.nice.org.uk/topics/male-pattern-baldness/ ↩
- Mella JM et al. “Efficacy and safety of finasteride therapy for androgenetic alopecia.” Arch Dermatol. 2010. DOI: 10.1001/archdermatol.2010.256 ↩
- Gupta AK, Charrette A. “Topical minoxidil for androgenetic alopecia.” Cochrane Database Syst Rev. DOI: 10.1002/14651858.CD007628 ↩
- Ludwig E. “Classification of the types of androgenetic alopecia (common baldness) occurring in the female sex.” Br J Dermatol. 1977. DOI: 10.1111/j.1365-2133.1977.tb15179.x ↩
- International Society of Hair Restoration Surgery — 2024 Practice Census and member directory. https://www.ishrs.org/ ↩
- General Medical Council — The Medical Register. https://www.gmc-uk.org/registration-and-licensing/the-medical-register ↩
How BergemHealth approaches this
Procedures are performed at JCI-accredited Liv Hospital Ulus, Istanbul, by Dr. Hamid Aydın and the resident surgical team. UK consultation and 12-month aftercare at our CQC-regulated Harley Street office. Transparent pricing and a free touch-up if indicated.
Free consultation →