Early Signs of Hair Loss: What to Look For at 25, 30, 35
Early signs of hair loss explained by age (25, 30, 35), how to tell a maturing hairline from a receding one, and four checks you can do at home.
Medical disclaimer. This article is educational and not medical advice. Hair restoration outcomes are individual; only a qualified clinician can assess your case in a personal consultation.
Quick answer
The two things most patients in their late 20s and early 30s confuse are a maturing hairline (normal adult transition where the temple corners recess slightly and evenly, often complete by 25–30) and early androgenetic alopecia (asymmetric, progressive, typically accompanied by miniaturisation). One needs no treatment; the other rewards early intervention. This guide covers age-specific patterns at 25, 30, and 35, four checks you can do at home, and when trichoscopy is genuinely useful.
Table of contents
- The age question: 25 vs 30 vs 35
- Maturing hairline vs receding hairline (the key distinction)
- Early signs at 25
- Early signs at 30
- Early signs at 35
- Four checks you can do at home
- When to see a clinician
- What you can do early
- How BergemHealth approaches early-stage assessment
- What to do next
- Frequently asked questions
The age question: 25 vs 30 vs 35
There’s no single “normal” hairline at any age — there’s a range, and the range shifts with age. What matters is change relative to your baseline, not comparison against an average.
Three rough age-cohort patterns are useful starting points. Roughly 16% of men aged 18–29 show some Norwood II–III recessionnice-mpb; by 30, that figure is 25–30%; by 35, around 35–40%. Early-onset AGA is genuinely common.
The right question at any of these ages isn’t “is my hairline normal?” — it’s “is my hairline changing, and if so in what pattern?”.
Maturing hairline vs receding hairline (the key distinction)
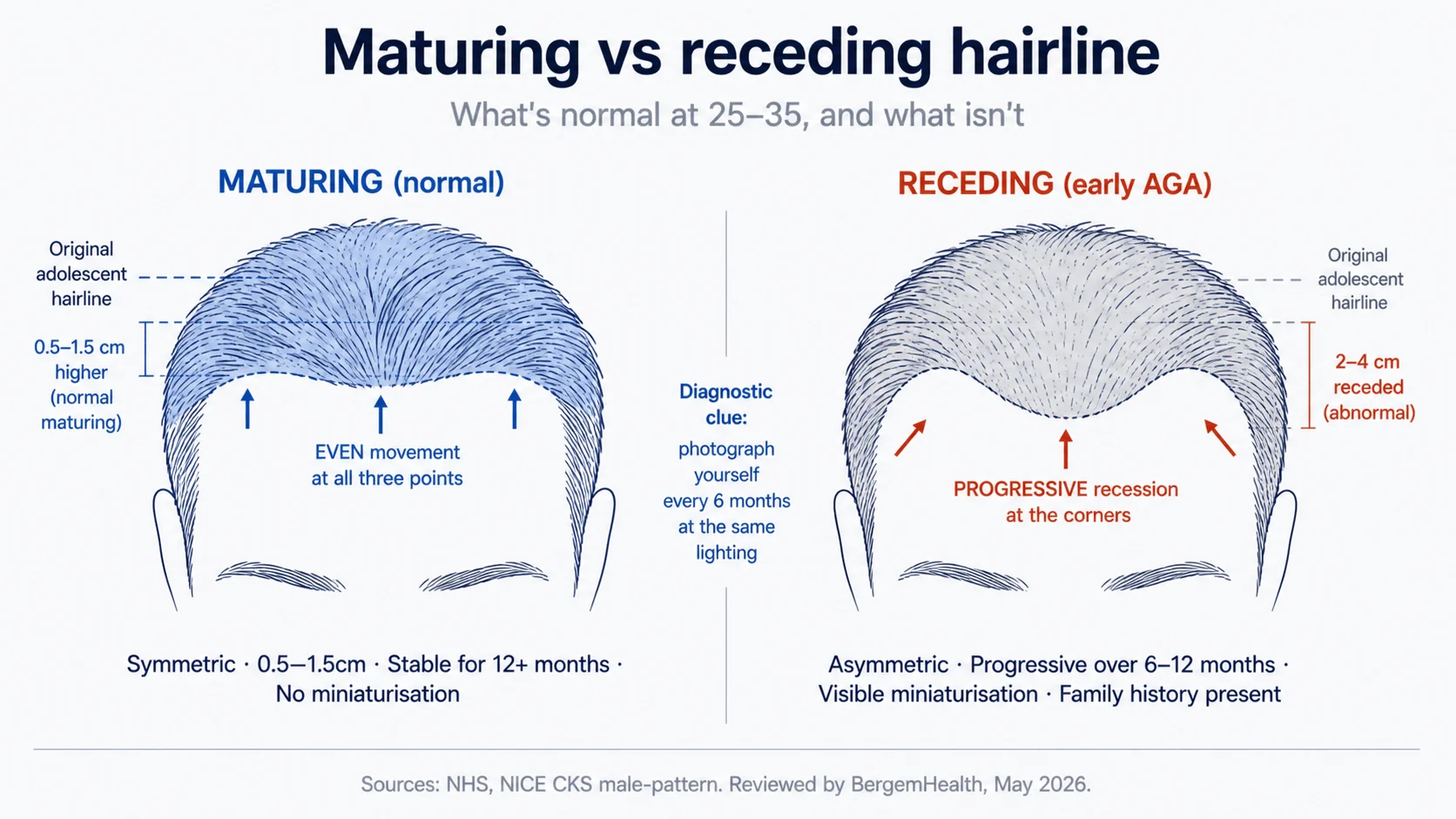
Definition. A maturing hairline is the normal adult transition from a low, rounded adolescent hairline to a slightly higher, less-rounded adult one — a small, even, bilateral recession at the temple corners, typically completing between 18 and 25. A receding hairline (early AGA) is asymmetric or progressive recession, often accompanied by hairs visibly thinner than surrounding hair (miniaturisation).
Maturing hairline: symmetric, small (0.5–1.5 cm above the adolescent line), stable once complete, no miniaturisation, late teens to early-mid 20s.
Early-AGA receding hairline: possibly asymmetric, progressive year by year, often deeper at the corners (M- or U-shape), miniaturisation visible (fine, lighter hairs in the receding zone), can occur at any age including 25 and earlier.
The distinction is genuinely difficult from a single photograph; trichoscopy distinguishes them by examining the hair shafts. If you’re unsure, photograph the hairline today and re-photograph in 12 months. A maturing hairline will look the same; an early-AGA hairline will look measurably different.
Early signs at 25
The most useful framing at 25: is the hairline still changing, or has it stabilised? Hairline maturation typically completes by 22–25, so changes at 25 not there at 22 are more likely early AGA than continued maturation.
Watch for: asymmetric temple recession; vertex thinning visible from above; miniaturised hairs at the front (fine, lighter, vellus-like); family history of advanced AGA on either side, particularly with 20s onset; shedding lasting >6 months without obvious trigger (temporary shedding 2–3 months after illness/stress is telogen effluvium, not AGA).
Earlier-onset AGA tends to predict more advanced eventual stages — identification at 25 is useful. Medical management started at 25 has more years to act before substantial miniaturisation accumulates.
Early signs at 30
At 30, AGA is recognisably common and the maturing-hairline question is mostly settled. The clinical question shifts from “is this happening?” to “what stage and trajectory?”.
Common features at 30: Norwood II–III recession in roughly 25–30% of mennice-mpb; crown thinning often visible to others before the patient sees it themselves; hair that feels finer or doesn’t hold style (miniaturisation visible before density loss is dramatic); more hairs on the pillow (volume is a poor diagnostic sign on its own).
Useful self-assessment at 30: three photographs in identical lighting (front, top-down, back-of-crown) compared with photos from 5 years ago. Five years of change tells you more than a single point-in-time view.
Early signs at 35
At 35, AGA prevalence in men of European ancestry is around 35–40%, and most men with AGA are at a clinically obvious stagenice-mpb. The questions at 35: what stage am I actually at (often slightly later than self-assessed); rate of progression over the last 5 years; whether to start medical management; whether it’s time for a hair-transplant assessment.
35 is often the age at which hair-transplant assessment first becomes useful — loss is established, trajectory is observable, and donor density is usually still good (it declines modestly with age).
Four checks you can do at home
Check 1: The standardised photo set. Photos in identical lighting and angle: front, top-down (parting visible), back-of-crown. Repeat every 6 months. Real change is visible across 12-month intervals; less reliable across 6 months because growth-cycle variation can mask small changes.
Check 2: The pull test. Gently grip 30–50 hairs near the scalp and slide outward with mild tension. Normal release is 1–2 hairs. More than 6 from a single grip suggests active sheddingtrichology. Repeat at 4–5 scalp locations. Non-specific but useful as an “is something happening” check.
Check 3: The miniaturisation check. Compare hairs in your receding zone (or along the parting) to hairs in the back-of-scalp donor zone. AGA-affected hairs are thinner, lighter, often shorter. A clear difference in shaft thickness between front and back means miniaturisation is happening. Phone-camera macro mode often works.
Check 4: The family-history check. Look at male relatives on both sides. Note pattern (typical Norwood vs Type A) and onset age. Not deterministic but strongly informative.
When to see a clinician
You don’t need a clinician to confirm a maturing hairline. See one if:
- You’re unsure whether it’s maturation or early AGA (30-minute trichoscopy resolves this)
- Shedding is heavy and lasting >6 months without identifiable trigger
- Sudden change rather than gradual progression
- Skin changes — redness, itching, scaling, pustules
- Hair loss is patchy rather than diffuse or patterned
- You’re considering medical management and want clinical assessment first
UK routes: GP first (initial assessment, blood work, possibly a referral), then trichologist or dermatologist (any case where scarring or inflammatory cause is suspected)nhstrichology. Hair-transplant clinics offer free pre-surgical assessments that include trichoscopy.
What you can do early
The earlier-stage your AGA, the more options. The realistic 2026 toolkit: finasteride, minoxidil topical 5% or low-dose oral, or both in combination. PRP is sometimes added as adjunct. Photographic monitoring every 6–12 months tracks response.
What’s not useful as primary therapy: over-the-counter “hair vitamins” without a documented deficiency, hair-loss shampoos with no active drug component, and direct-to-consumer wellness supplements. None have evidence comparable to finasteride or minoxidil.
How BergemHealth approaches early-stage assessment
Most early-stage patients aren’t looking for surgery — they’re looking for an honest answer to “do I have AGA, and what should I do now?”. The free initial consultation (at Harley Street or by video) covers clinical history, trichoscopy of frontal/parting/donor regions, donor-density measurement, and a discussion of which treatment tier is right for the current stage.
For early-stage patients (Norwood II–III equivalent), the recommendation is medical management first — finasteride and/or minoxidil, reviewed at 12 months. Surgery becomes a sensible conversation later, if and when the trajectory progresses beyond what medical management stabilises. Telling a 25-year-old at Norwood II that a transplant is the wrong tool right now is part of the assessment.
Per-graft pricing, when surgery eventually becomes appropriate, is the same on both sides: from £1,250 (Standard FUE), £1,750 (Sapphire FUE), £2,250 (Direct DHI). Surgery happens at Liv Hospital Ulus (Istanbul, JCI-accredited) or 99 Harley Street (London, CQC-registered) — logistical choice. Dr. Sumeyye Yuksel leads the GMC-registered consulting team at Harley Streetgmc; the surgical pathway in Istanbul is led by Dr. Hamid Aydın (ISHRS, 25,000+ procedures)ishrs.
What to do next
If you want to understand what’s happening, the AGA article covers the mechanism and lookalikes; the Norwood walkthrough helps with self-staging. For broader context: the Hair Loss pillar.
If you’re ready to start medical management, see the finasteride and minoxidil articles and speak to your GP.
If you want a trichoscopy assessment to confirm what you’re seeing, request a free assessment from BergemHealth’s London or Istanbul team.
Frequently asked questions
Is it normal to lose hair in your 20s?
Roughly 16% of men aged 18–29 show some Norwood II–III recessionnice-mpb. Early-20s hair loss is genuinely common — neither rare to dismiss nor universal to assume. The clinical question isn’t whether it’s “normal” but whether it’s likely to progress and whether early medical management is appropriate.
How can I tell if my hairline is maturing or receding?
A maturing hairline is symmetric, small (0.5–1.5 cm above the adolescent line), and stable once complete. A receding hairline is often asymmetric, progressive, and accompanied by miniaturised hairs. The most reliable home test is photographic comparison every 12 months — a maturing hairline doesn’t change after maturation completes; an AGA hairline measurably progresses.
How many hairs a day is normal to lose?
Adults shed roughly 50–100 hairs per day as part of normal hair-cyclingnhs. The number varies with washing frequency, season, and stress. The “100 hairs a day” rule is reassurance for short-term shedding worry, not a diagnostic test. Volume isn’t a sensitive indicator — pattern and miniaturisation are.
Should I start finasteride at 25 if I’m at Norwood II?
An individual decision worth discussing with a GP. The case for early start: medical management works better before substantial miniaturisation, and starting at 25 gives 5+ years of action before reaching Norwood III–IV. The case for waiting: side-effect risk is real, visible benefit at Norwood II is small, and you can always start later. Side-effect data in the finasteride article.
Does drinking, smoking, or diet affect early hair loss?
Severe nutritional deficiency can cause shedding (typically telogen effluvium, not AGA). Heavy smoking has weak links to AGA progression in some studies; the effect, if real, is small. Alcohol within normal limits is unlikely to matter. Most actionable lifestyle factors: stress management and avoiding rapid weight loss.
If both my parents have full hair, can I still go bald?
Yes. AGA is multi-genic and partially environmental; family history is informative but not deterministic. Personal observation of your trajectory is more informative than family history alone.
How quickly should I see results from finasteride or minoxidil?
Both require 4–6 months for visible effect, 12 months for reasonable assessmentmella-fincochrane-min. Minoxidil’s first 8–12 weeks can include a “shedding phase” — normal, not failure. Finasteride usually doesn’t. Consistent daily use is how both drugs work.
Can a hair transplant be done at 25?
Generally no — and a defensible clinic will say so. AGA progression is still active and unpredictable at 25, a transplanted hairline can become an isolated island as surrounding hair recedes, donor density should be preserved, and medical management often hasn’t been adequately tried. Exceptional reconstructive cases exist, but routine elective AGA surgery at 25 is best deferred.
Sources
- NHS — Hair loss overview. https://www.nhs.uk/conditions/hair-loss/ ↩
- NICE Clinical Knowledge Summary — Male pattern baldness. https://cks.nice.org.uk/topics/male-pattern-baldness/ ↩
- StatPearls — Androgenetic Alopecia. National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK430924/ ↩
- Institute of Trichologists (UK) — Position statements. https://www.trichologists.org.uk/ ↩
- Mella JM et al. “Efficacy and safety of finasteride therapy for androgenetic alopecia.” Arch Dermatol. 2010. DOI: 10.1001/archdermatol.2010.256 ↩
- Gupta AK, Charrette A. “Topical minoxidil for androgenetic alopecia.” Cochrane Database Syst Rev. DOI: 10.1002/14651858.CD007628 ↩
- International Society of Hair Restoration Surgery — 2024 Practice Census and member directory. https://www.ishrs.org/ ↩
- General Medical Council — The Medical Register. https://www.gmc-uk.org/registration-and-licensing/the-medical-register ↩
How BergemHealth approaches this
Procedures are performed at JCI-accredited Liv Hospital Ulus, Istanbul, by Dr. Hamid Aydın and the resident surgical team. UK consultation and 12-month aftercare at our CQC-regulated Harley Street office. Transparent pricing and a free touch-up if indicated.
Free consultation →